
With occiput posterior and spine anterior position on ultrasound, none of the babies was born in the occiput posterior position. 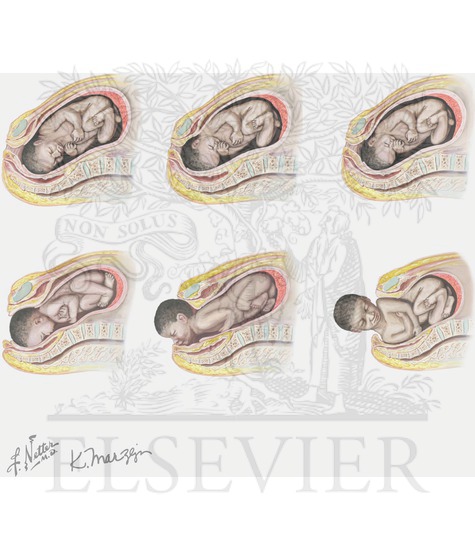
There were 6 cases of occiput posterior position at delivery all of these were among the 23 fetuses in an occiput posterior position during the second stage of labor. The rate of occiput posterior position during the first stage of labor was 51%, but the majority of these cases rotated to an anterior position before delivery. In their prospective cohort study, 100 singleton pregnant women underwent intrapartum ultrasound during the first and second stages of labor, and the positions of the fetal head and spine were defined. 
suggest that the positions of the head and spine during the second stage of labor could be practical indicators for predicting the occiput posterior position at delivery. Several recent studies support this notion of POPP as the main cause of occiput posterior delivery, although the concept of malrotation of the initial occiput anterior or transverse position for POPP prevailed even until approximately a decade ago. Nevertheless, most occiput posterior positions at delivery are the initial occiput posterior position rather than misrotation from an original occiput anterior or transverse position. Occiput posterior position during labor mostly changes to the anterior position even at full cervical dilatation. POPP is associated with approximately 4- and 13-fold higher rates of operative vaginal and cesarean deliveries, respectively. POPP is a well-known cause of abnormal labor and occurs in approximately 5% of deliveries and 20% at labor onset. The main reason for using sonography to define fetal position is to diagnose persistent occiput posterior position (POPP). Nevertheless, the discordance rate between vaginal examination and ultrasound assessment was also high (76%) during active labor. However, during active labor, attending physicians were almost twice as successful at measuring the correct fetal head position by physical examination. Interestingly, in that study, there was no difference in the technique of senior residents and attending physicians. Similarly, another study of 112 patients in the second-stage of labor at term with normal single cephalic-presenting fetuses and membrane rupture demonstrated a high rate of error (65%) of the vaginal digital assessment of fetal head position compared to ultrasound assessment as the gold standard. In a study of 496 single pregnancies in labor at term, digital examination failed to detect the fetal head position in 166 cases (33.5%) moreover, the digital and sonographic findings were concordant in only 163 cases. Regarding cardinal movement, ultrasound examination may provide more accurate information about fetal position than digital examination. In this review, we discuss the usefulness of intrapartum ultrasound for the evaluation of labor progress and predicting successful operative vaginal delivery.ĭuring labor, the fetus exhibits the cardinal movements of labor, which include engagement, descent, flexion, internal rotation, extension, external rotation, and expulsion. abnormal labor, the specific targets of intrapartum ultrasound are the engagement of the fetal head into the maternal pelvis, fetal head station, the detection of occiput posterior position during labor, and placental separation. Therefore, it remains to be determined if intrapartum ultrasound can be used to diagnose the presence of abnormal labor and predict the possibility of successful instrumental delivery, consequently improving maternal and fetal outcomes.Īs determinants of normal vs. The incidence of intracranial hemorrhage with cesarean section following failed operative vaginal delivery is 1/334 compared to 1/860 with successful vacuum delivery. Furthermore, cesarean section after failed vacuum extraction is also associated with an increased risk of fetal trauma. Because the fetal head is impacted deeply in the maternal pelvis, second-stage cesarean section is in association with increased maternal risks such as major hemorrhage, bladder injury, and extension tears of the uterine angle resulting in broad ligament hematoma. For the fetus successful instrumental delivery is safer than emergency cesarean delivery. When progress failure or fetal distress occurs, obstetricians should choose between an operative vaginal delivery or a cesarean section. Although most obstetric ultrasound examinations are performed to make antenatal diagnoses of fetal abnormalities, the use of ultrasound for women in labor is increasing as a result of accumulating evidence of its usefulness for objectively evaluating the progress of labor.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
